Hair Loss Treatment
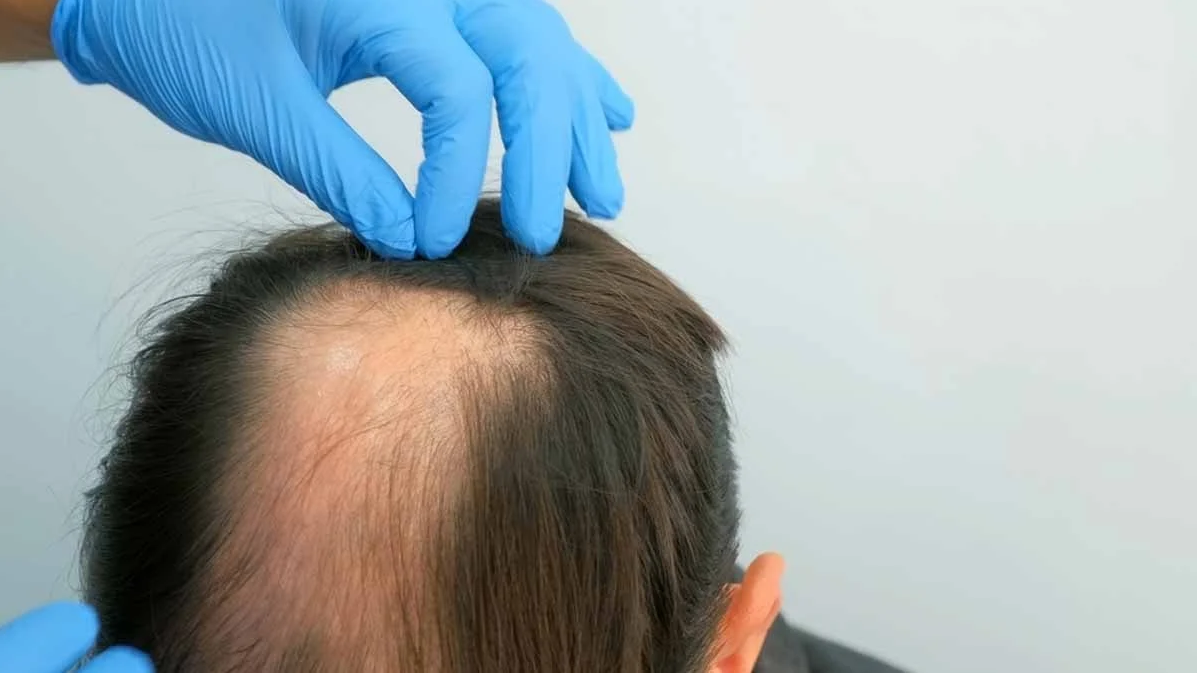
Hair loss (alopecia) differential diagnosis (causes) involves distinguishing between non-scarring (reversible) and scarring (permanent) types based on pattern, inflammation, and hair pull test results. Common causes include androgenetic alopecia, telogen effluvium, alopecia areata, and traction alopecia, requiring evaluation of medical history, hair care practices, and potential scalp biopsy (this would require a referral to Dermatology).
Key Differential Categories
- Non-Scarring Alopecia (Most Common):
- Androgenetic Alopecia: Patterned hair loss (vertex thinning or bitemporal recession in men; diffuse crown thinning in women).
- Telogen Effluvium: Sudden, diffuse shedding often triggered by stress, illness, childbirth, or severe weight loss.
- Alopecia Areata: Autoimmune condition causing smooth, round, coin-like patches of hair loss.
- Traction Alopecia: Gradual hair loss along the hairline caused by tight hairstyles, commonly associated with a “fringe sign”.
- Trichotillomania: Impulse control disorder leading to hair pulling, often with broken hairs of varying lengths.
- Tinea Capitis: Fungal infection causing scaly, erythematous patches, often in children.
- Anagen Effluvium: Sudden loss due to chemotherapy or severe radiation.
Scarring (Cicatricial) Alopecia (Irreversible):
- Lichen Planopilaris: Often presents with perifollicular erythema (redness) and scaling.
- Central Centrifugal Cicatricial Alopecia (CCCA): Usually starts at the vertex (crown), often affecting black women.
- Discoid Lupus Erythematosus (DLE): Inflammatory skin disease with scarring.
- Folliculitis Decalvans: Type of neutrophilic scarring hair loss.
Diagnostic Workup
• Physical Exam: Note the pattern (diffuse or patchy), presence of hair follicles (absent in scarring), and scalp inflammation.
• Hair Pull Test: More than 10% of hair pulled indicates active shed (positive in telogen effluvium).
• Laboratory Tests: Check thyroid function (TSH), iron levels (ferritin), Vitamin B12, Vitamin D, and zinc, especially if hair loss is diffuse.
• Scalp Biopsy: Needed to confirm scarring subtypes (requires Dermatology referral)
Causes to Rule Out
• Endocrine Issues: Thyroid disease (hyper/hypothyroidism), PCOS.
• Nutritional Deficiencies: Lack of Vitamin B12, Biotin (Vitamin B7), iron (ferritin), zinc, protein, or vitamin D.
• Medications/Illness: Recent shocks to system: child-birth, surgery, high fever, or new medications
• Infection: STDs (Syphilis), Fungal infections like Ringworm, MRSA, Viral infections such as COVID, Varicella (Chicken pox or Shingles), EBV (Mono) can induce telogen effluvium.
• Autoimmune phenomenon: Rheumatoid Arthritis, Lupus, Sjogren’s syndrome
FDA – Approved Medication for Men
The FDA has approved only two medications for the direct treatment of male pattern hair loss (androgenetic alopecia). These are considered the “gold standard” of medical management and are most effective when started early. Primary Addiction Medicine Care of Connecticut feels comfortable and confident prescribing these medications to men for hair loss.
1. FDA-Approved Medications
• Finasteride (Brand: Propecia):
- Form: A 1 mg oral pill taken once daily.
- Mechanism: It is a DHT blocker that inhibits the enzyme (Type II 5-alpha-reductase) responsible for shrinking hair follicles.
- Efficacy: Highly effective at slowing hair loss and potentially promoting regrowth, especially at the crown (vertex).
- Availability: Requires a prescription from a healthcare provider.
- Topical Minoxidil (Brand: Rogaine):
- Form: Liquid or foam applied directly to the scalp, typically twice daily.
- Mechanism: A vasodilator that stimulates blood flow and prolongs the growth (anagen) phase of hair follicles.
- Efficacy: Available in 2% and 5% strengths; the 5% strength is more effective for men.
- Availability: Over the counter (OTC) and oral tablet requires prescription
FDA – Approved Medication for Women
For women experiencing hair loss, specifically female pattern hair loss (androgenetic alopecia), the FDA has approved one primary medication and cleared several medical devices as of early 2026.
1. FDA-Approved Medication
Topical Minoxidil (brand name Rogaine) is the only medication specifically FDA-approved for female hair loss.
- • Formulations: It is available over the counter in two strengths:
- 2% Topical Solution: Usually applied twice daily.
- 5% Topical Foam: FDA-approved for women in 2014 for once-daily use.
- Effectiveness: Studies show roughly 60% of women see results, with visible improvement typically taking 6–12 months of consistent use.
2. FDA-Cleared Devices
Low-Level Laser Therapy (LLLT) devices are “FDA-cleared” (a different regulatory standard than “approved”) for treating female pattern thinning. These devices use red light to stimulate hair follicles at a cellular level.
• Common Forms: These are available as home-use laser caps, helmets, and combs.
• Examples: Brands like Hairmax, iRestore, and Theradome offer cleared products.
3. Off-Label Treatments (Commonly Prescribed)
Many doctors prescribe medications “off-label,” meaning they are FDA-approved for other conditions but have scientific backing for hair loss. Primary Addiction Medicine Care of Connecticut feels comfortable prescribing the following medication to women for hair loss including:
• Oral Spironolactone: A diuretic approved for high blood pressure but widely used for its anti-androgen effects to treat hormonal thinning in women.
• Low-Dose Oral Minoxidil: A pill form of minoxidil that is often used when topical versions are too messy or irritating.
• Finasteride/Dutasteride: Though FDA-approved for men, these are sometimes prescribed for post-menopausal women.
